THESIS REPORT
The role of health literacy in osteoporosis prevention
Sarah Hosking
November 2019
Introduction: Osteoporosis and associated fragility fractures are increasing in prevalence and they are costly both in terms of financial costs to the healthcare system and personal costs associated with reduced independence and quality of life for the individual. Lifestyle recommendations for the prevention of osteoporosis have previously been developed and include guidelines for consuming adequate dietary calcium, ensuring adequate levels of vitamin D, limiting alcohol intake, avoiding smoking and undertaking weight bearing physical activity. However, these recommendations are not universally taken up or adhered to. Previous research has reported a relationship between low health literacy and poor uptake of prevention behaviours in other chronic diseases; however, research regarding health literacy and prevention of osteoporosis is currently lacking. Thus, the overarching aim of this thesis was to investigate potential associations between health literacy in women and osteoporosis prevention. Health literacy data were collected using the multidimensional Health Literacy Questionnaire (HLQ), for women participating in the Geelong Osteoporosis Study (GOS) from December 2014 to March 2016 and for women participating in the 11 year follow-up of the Vitamin D in Pregnancy (VIP) Study from 2013 to 2016. Additional data regarding sociodemographic characteristics, osteoporosis prevention behaviours and a diagnosis of osteoporosis according to self-report and bone mineral density (BMD) criteria, were collected for women at the 15 year follow-up of the GOS from 2011 to 2014. Mothers in the VIP study also provided sociodemographic data and information regarding maternal and child osteoporosis prevention behaviours. Analyses were undertaken to determine if health literacy scores differed between: women who adhered to osteoporosis prevention recommendations compared to those who did not, women who correctly self-reported osteoporosis status compared to those who did not, and mothers of children who participated in activities which promoted bone health compared to mothers of children who did not. Analysis of variance was used to determine inter-group differences in health literacy scores, and effect sizes were calculated using Cohen’s D to determine the magnitude of differences between groups. Regression analyses were undertaken to investigate associations between health literacy and sociodemographic characteristics and to determine the relationship between sociodemographic characteristics, health literacy and osteoporosis prevention behaviours.
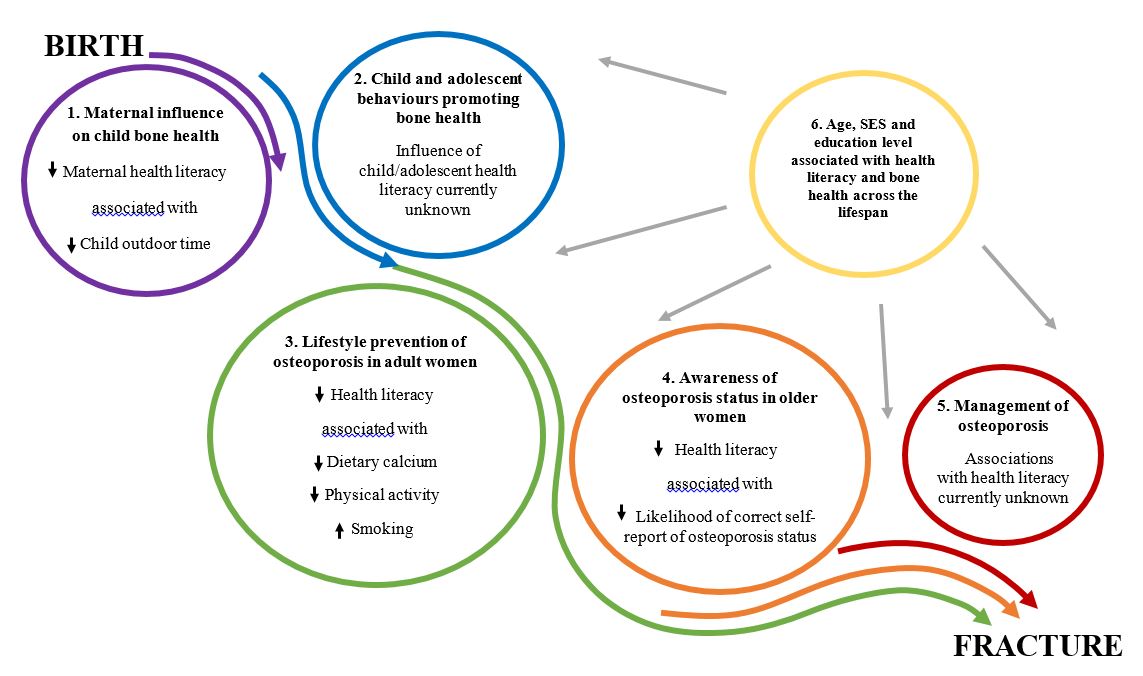
Results: In GOS women, lower health literacy scores were associated with older age, lower socioeconomic status (SES) and lower level of education. Additionally, lower health literacy scores were associated with inadequate dietary calcium intake, decreased physical activity levels and increased likelihood of smoking. Higher health literacy scores were associated with alcohol intakes above recommended levels, however, this association was attenuated by age and was likely explained by the inverse relationship between age and health literacy. No data were collected on vitamin D status. In older GOS women, lower health literacy scores were associated with a self-reported osteoporosis status that did not match BMD diagnosis of osteoporosis with the majority of women self-reporting no osteoporosis despite having met criteria for a clinical diagnosis of osteoporosis. Finally, lower maternal health literacy was associated with decreased outdoor time but not calcium intake or screen time in children. For mothers, a trend was observed for a relationship lower health literacy and smoking but not dietary calcium or alcohol intake.
Conclusion: Together, these findings suggest that the health literacy of women may play a role in their ability to understand and adhere to osteoporosis recommendations, encourage behaviours that support bone health in their children, and recognise their own osteoporosis status. Health literacy should be a consideration in future initiatives to convey osteoporosis prevention recommendations to the wider community and in communicating a diagnosis of osteoporosis within a healthcare setting.
Full text of Dr S. Hosking’s thesis is available from HERE

Sarah Hosking, PhD
Deakin University, Australia.

