THESIS REPORT
Characterization of T cells in Bone Metastasis from Breast Cancer for Immunotherapeutic Treatment
Danna L. Arellano
April 2020
Bone metastases occur when cancer cells disseminate from the primary to the bones, and they are a frequent complication in patients with advanced-stage breast or prostate cancer. Skeletal metastases disrupt bone remodeling, causing fractures or nerve compression, and reducing the quality of life of patients with pain or paralysis. Current treatments like bisphosphonates can protect from these skeletal complications but do not cure patients. Therefore, it is important to look for new therapeutic strategies like immunotherapy.
Immunotherapy uses elements of the immune systems, such as antibodies, or the own immune system of patients, such as T cells, to eliminate cancer cells. It has been approved for the treatment of different types of cancers and is still tested for many others in clinical trials, but not for bone metastases so far. A potential limiting factor for the use of immunotherapy and T cells with bone metastases is the ability of T cells to increase bone resorption, as observed in rheumatoid arthritis or osteoporosis, which could support bone metastases.
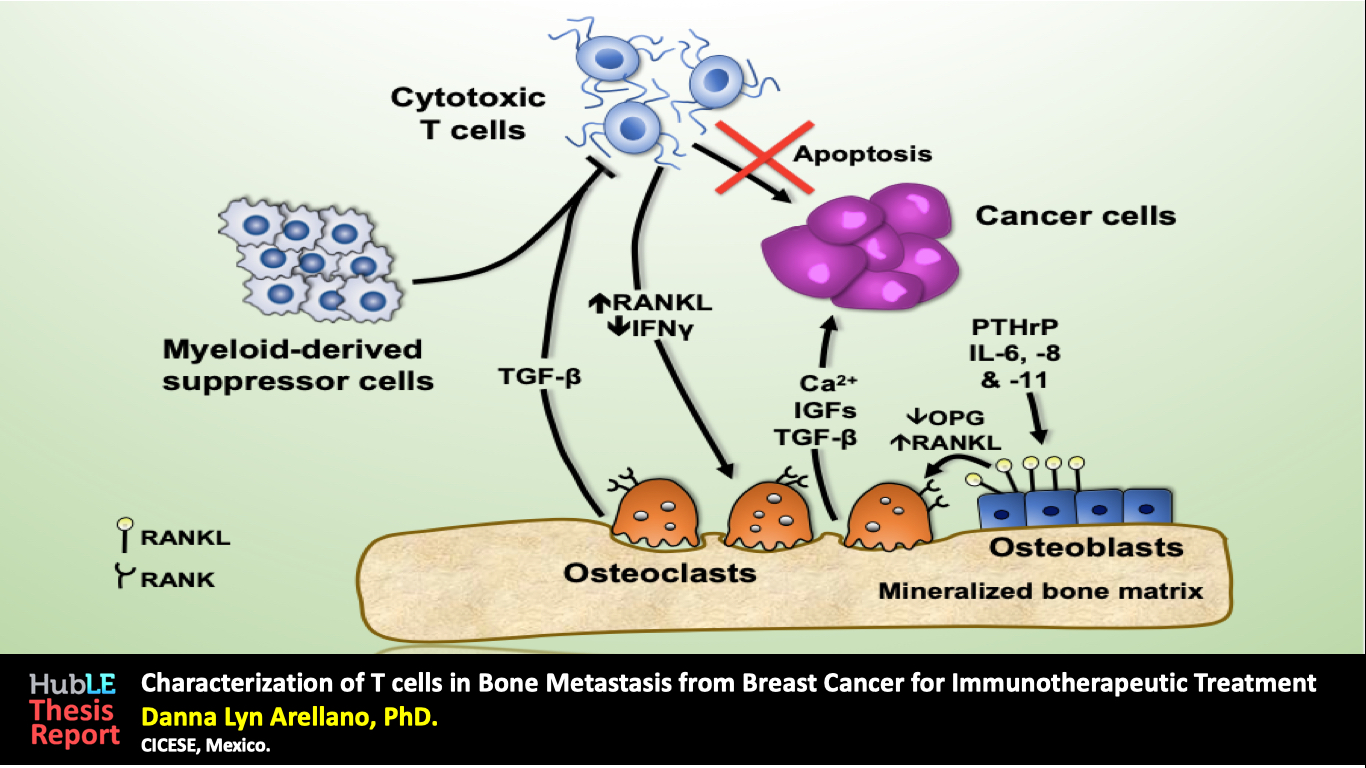
Using a syngeneic mouse model of bone metastases from breast cancer, we demonstrated that the absence of T cells in SCID or T cell-depleted mice decreased the number of osteoclasts in the tumor microenvironment, as well as the development of bone metastases. Consistently, T cells increased the formation of osteoclasts in bone marrow co-culture ex vivo, but only when they were not activated. Analysis of expression of activation markers using flow cytometry confirmed that T cells were not activated in bone metastases. Such lack of activation could be due to an accumulation, in the bone marrow, of myeloid-derived suppressor cells (MDSCs) that express inhibitors of T cells such as reactive oxygen species (ROS), nitric oxide (NO), or immune checkpoint proteins. In sharp contrast, upon activation ex vivo, the properties of T cells changed, and they turned into inhibitors of the formation of osteoclasts.
Therefore, our results suggest that T cells are inactivated in bone metastases and increasing them by inducing the formation of osteoclasts and bone resorption. These results also suggest that activating T cells with immunotherapy could not only increase their anti-cancer effect but also inhibit cancer cell-induced bone resorption to benefit patients suffering from bone metastases.
Full text of D. Arellano’s thesis is unavailable.

Danna Lyn Arellano, PhD
Center of Scientific Research and Higher Education at Ensenada (CICESE), B.C. Mexico.